By Lauren R. Rosecan, M.D., Ph.D., F.A.C.S.
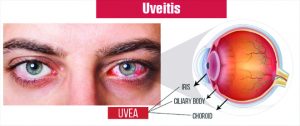 Uveitis is inflammation of the uvea, which is made up of the iris, ciliary body and choroid. Together, these form the middle layer of the eye between the retina and the sclera (white of the eye).
Uveitis is inflammation of the uvea, which is made up of the iris, ciliary body and choroid. Together, these form the middle layer of the eye between the retina and the sclera (white of the eye).
The eye is shaped like a tennis ball, with three different layers of tissue surrounding the central gel-filled cavity, which is called the vitreous. The innermost layer is the retina, which senses light and helps to send images to your brain. The outermost layer is the sclera, the strong white wall of the eye. The middle layer between the sclera and retina is called the uvea.
The uvea contains many blood vessels — the veins, arteries and capillaries — that carry blood to and from the eye. Because the uvea nourishes many important parts of the eye (such as the retina), inflammation of the uvea can damage your sight.
There are several types of uveitis, defined by the part of the eye where it occurs.
Iritis affects the front of your eye. Also called anterior uveitis, this is the most common type of uveitis. Iritis usually develops suddenly and may last six to eight weeks. Some types of anterior uveitis can be chronic or recurrent.
If the uvea is inflamed in the middle or intermediate region of the eye, it is called pars planitis (or intermediate uveitis). Episodes of pars planitis can last between a few weeks to years. The disease goes through cycles of getting better, then worse.
Posterior uveitis affects the back parts of your eye. Posterior uveitis can develop slowly and often lasts for many years.
Panuveitis occurs when all layers of the uvea are inflamed.
Uveitis Causes
The specific cause of uveitis often remains unknown. In some cases, however, it can be associated with other disease or infection in the body.
Uveitis may be associated with:
- A virus, such as shingles, mumps or herpes simplex;
- Systemic inflammatory diseases;
- A result of injury to the eye; or
- Rarely, a fungus, such as histoplasmosis or
- a parasite, such as toxoplasmosis.
If you smoke, stop. Studies have shown that smoking contributes to the likelihood of developing uveitis.
Uveitis Symptoms
Uveitis may develop suddenly with eye redness and pain, or with a painless blurring of your vision. In addition to red eye and eye pain, other symptoms of uveitis may include light sensitivity, blurred vision, decreased vision and floaters. There may also be a whitish area (called a hypopyon) obscuring the lower part of the iris.
A case of simple “red eye” may in fact be a serious problem such as uveitis. If your eye becomes red or painful, you should be examined and treated by an ophthalmologist .
Uveitis Diagnosis
A careful eye examination by an ophthalmologist is extremely important when symptoms occur. Inflammation inside the eye can permanently affect sight or even lead to blindness if it is
not treated.
Your ophthalmologist will examine the inside of your eye. He or she may order blood tests, skin tests or X-rays to help make the diagnosis.
Since uveitis can be associated with disease in other parts of the body, your ophthalmologist will want to know about your overall health. He or she may want to consult with your primary care physician or other medical specialists. However, in approximately 40 to 60 percent of cases, no associated disease can be identified.
Uveitis Treatment
Uveitis is a serious eye condition that may scar the eye. It needs to be treated as soon as possible. Eyedrops, especially corticosteroids and pupil dilators, can reduce inflammation and pain. For more severe inflammation, oral medication or injections may be necessary.
If left untreated, uveitis may lead to:
- Glaucoma (increased pressure in the eye);
- Cataract (clouding of the eye’s natural lens);
- Neovascularization (growth of new, abnormal blood vessels); or
- Damage to the retina, including retinal detachment, damage to the optic nerve or both.
These complications may also need treatment with eye drops, conventional surgery or laser surgery. If you have a “red eye” that does not clear up quickly, contact your ophthalmologist.
Lauren R. Rosecan
M.D., Ph.D., F.A.C.S.
The Retina Institute of Florida with four offices conveniently located in Palm Beach and Martin Counties.
Toll Free Phone Number: 1-800-445-8898 561-832-4411
West Palm Beach
901 North Flagler Drive, 33401
(561) 832-4411 Office
(561) 832-1591 Fax
Palm Beach Gardens
11382 Prosperity Farms Rd., #128, 33410
(561) 627-7311 Office
(561) 627-6791 Fax
Stuart
618 East Ocean Blvd., #3, 34994
(772) 287-7026 Office
(772) 220-4186 Fax
Boca Raton
1050 NW 15th Street, #114, 33486
(561) 368-7723 Office
(561) 368-0093 Fax
 South Florida Health and Wellness Magazine Health and Wellness Articles
South Florida Health and Wellness Magazine Health and Wellness Articles




