By Matthew Stiebel, MD, FRCSC –
Q: What do Drew Brees, Lamar Odom, and Jacoby Ellsbury all have in common?
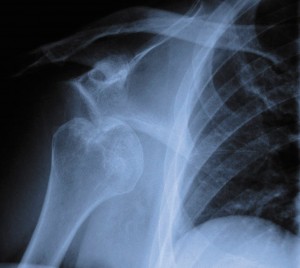 A: Yes, they are all professional athletes, and they all have an annual income just slightly below the GDP of Bolivia, but (more to my point) they have all dislocated their shoulder at one time or another.
A: Yes, they are all professional athletes, and they all have an annual income just slightly below the GDP of Bolivia, but (more to my point) they have all dislocated their shoulder at one time or another.
The easiest way to think of the shoulder joint is to imagine a golf ball on a tee. The golf ball is the head of the humerus bone and the glenoid is the socket or the tee. Much like an actual tee, the glenoid is a very small structure when compared to the size of the head of the humerus. The head of the humerus is therefore stabilized on the glenoid by a number of supporting actors. These players include the rotator cuff, the joint capsule, a few ligaments, and most importantly the labrum. The labrum is a tough rubber bumper/ gasket made of cartilage that helps keep the humeral head centered in the glenoid. Often when a shoulder is dislocated, (when the golf ball falls off of the tee) the tough labral tissue gets ripped off of the glenoid. This means that even after the golf ball is relocated on the tee (the shoulder is put back in joint) it has a higher rate of falling off/ dislocating again because it lacks the stabilizing force of the labrum. This means that even though the first event to dislocate the shoulder might have been a huge trauma, the shoulder may dislocate again with much smaller forces. It therefore becomes less likely to remain in joint and is effectively “unstable”…. Not unlike some of the people you meet at Wal Mart at 3 am….
Interestingly, young athletes under the age of 18 have an almost 80% rate of re-dislocation after their first event! This means that they are more likely to need a surgical reconstruction of the labrum than older patients. Shoulders that dislocate may require some assistance to keep the humerus centered on the glenoid. Often an orthopaedic surgeon will re-attach the labrum to the bone of the glenoid with sutures and tiny anchors and tighten up the capsule around the joint. This type of injury is so common that it’s named after the surgeon who ‘discovered’ it: Arthur Sydney Blundell Bankart. It is known as a “Bankart repair” to correct the detached labrum (the Bankart lesion.) Some weird pride usually makes us doctors want to name things after ourselves… just ask Dr Syphilis how his kids feel about that.
As technology has advanced we, as surgeons, have gotten more adept at treating unstable shoulders. We have all sorts of fancy new gadgets that allow us to operate minimally invasively with the arthroscope, and we have newer and stronger sutures and bone anchors that give us more solid repairs. Also, perhaps even more importantly, we have learned more about different types of shoulder dislocations.
We have begun to classify dislocations in terms of the direction they dislocate (to the front of the body, or to the back, or both), we have identified different types of concurrent bone lesions (such as the breaking of the golf tee or the denting of the golfball) and we have developed newer techniques to fix these defects. In essence, we are moving in the right direction in terms of shoulder reconstruction and are, in this author’s opinion, rapidly entering the golden age of arthroscopic shoulder reconstruction. So, there’s never been a better time in history to dislocate that shoulder—and then to get it fixed. My advice is to keep up with that wild arm swinging in your Insanity workout or Crossfit gym and remember to keep the Palm Beach Sportsmedicine appointments number on speed dial… Now if only I can identify that soon to be historic “Stiebel lesion….”
Matthew Stiebel, M.D. FRCSC
Board Certified, Fellowship Trained Orthopaedic Surgeon
Matthew Stiebel, MD FRCSC, is the newest partner at Palm Beach Sportsmedicine. After un-
dergraduate and medical school degrees at Yale University, he completed an orthopaedic surgery residency at McGill University and a subspecialty fellowship in sports medicine at Boston University. His specialties include complex shoulder and knee injuries. Dr Stiebel has published papers and book chapters on specialty surgeries of the knee and shoulder. He is an associate master instructor for the Arthroscopy Asscociation of North America, where he instructs both arthrocopic shoulder and patellofemoral knee courses for surgeons in the US and internationally. He has lectured to the International Patellofemoral Reseach Group in London and New York City, and has worked with patellofemoral implant design companies. His other current interest involves the repair of pectoralis major muscle tears and their subsequent outcomes. While in Montreal, Dr Stiebel worked with the Montreal Canadians Hockey team and Expos Baseball team. During his fellowship time in Boston he was able to serve as team physician for the NCAA championship BU men’s hockey team, UMASS Boston Hockey, as well as work with the World Wrestling Entertainment Summer Slam Series. Locally, Dr Stiebel stays active in the community by currently serving as team physician for some of the local high school football and gymnastics programs.
Certificates/Memberships:
– Board Certification: American Board of Orthopaedic Surgery, July 2012
– American Academy of Orthopaedic Surgeons
– Fellow, Royal College of Physicians and Surgeons of Canada American Arthroscopy Association of North America
– International Society of Arthrosocopy, Knee Surgery & Orthopaedic Sports Medicine
– International Patellofemoral Reseach Group
Palm Beach Sport Medicine
(561) 845-6000
www.pbsportsmed.com
Check Also
The Latest Technology With Hearing Aids
Many modern electronic devices these days come equipped with Bluetooth technology. This feature lets you …
 South Florida Health and Wellness Magazine Health and Wellness Articles
South Florida Health and Wellness Magazine Health and Wellness Articles