By Matthew Stiebel, MD, FRCSC –
“The six million dollar man ain’t got nothing on me, Doc!”
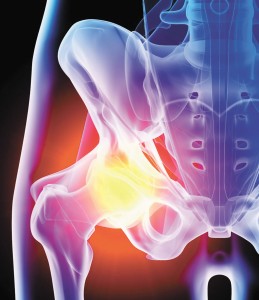 According to the CDC, arthritis (aka. worn out joint cartilage) is the leading cause of disability in the United States.
According to the CDC, arthritis (aka. worn out joint cartilage) is the leading cause of disability in the United States.
Over 43 million people suffer from pain due to arthritic joints. While over 800,000 joint replacements were performed in 2003, with the baby boom approaching 65 and older—that number is expected to grow to well over one million joints per annum in the next few years. Clearly, we are approaching a society where a significant portion of the population will have some form of metal joints….And you thought that limbs from the Terminator were only the stuff of science fiction?
While modern joint replacements have been around since the 1970’s, technologies have changed drastically with regards to metallurgy and plastic polymerization techniques in the last few years. Today joints are expected to last between 15 and 20 years depending on the demands placed on them. Additionally, the most exciting changes in joint replacement are now coming from deeper understandings of body mechanics. With better computational models and more sophisticated techniques to measure joint rotation and stability, we are designing smaller, partial joints and more anatomically correct complete joints for replacement. These joints take much less stress than the older, less anatomical designs, and therefore have much greater longevity. Additionally, now we can tailor joints much more specifically for the patient and the disease pattern. (Think of a bespoke suit instead of an off the rack job.)
As a surgeon, I have a much greater toolbox than ever before (instead of just one hammer looking for nails). I can treat cartilage lesions with everything from cartilage transplants, to bony realignments, to small metal partial replacements, to partial total joints, all the way up to full total replacements– depending on the age, activity and expectations of the patient. Whereas before, total joints were the only option for patients with arthritis and pain, now we have a much greater armamentarium to customize options for patients. Through this customization, arthritis patients can remain as active as possible. In fact, many patients that come to me expecting total joint replacements are often pleasantly surprised when I explain to them that a smaller, less invasive surgery is often a much better option.
What’s next for the world of joint replacement you ask? Longevities greater than 20 years? Artificial parts that are computer designed specifically for me? Less invasive surgeries with computer guidance and shorter recoveries? Well, actually—all of these things are currently being utilized today and are staples of our practice right here in Jupiter and West Pam Beach…. But the biggest objective on the horizon is not actually a change in the total joint itself—but it may be in preventing them.
If we could “repaint” joints with that smooth slippery Teflon cartilage that they lost while becoming arthritic—then we wouldn’t need metal and plastic. Unfortunately this “spray paint cartilage” may be 20-30 years away. (Yes, as a solid blow to my ego I realize that the greatest advancements in medicine over the next century will probably come from engineers and not actually from doctors- despite what I thought when I entered medical school.) But, until that time when we have truly effective cartilage replacements—current techniques with resurfacings, partial or even total joint replacements are our very best options. And while they may not take strokes off of your golf game, they most assuredly will let you get back out on the links or the tennis courts with significantly less pain.
Matthew Stiebel, M.D. FRCSC
Board Certified, Fellowship Trained Orthopaedic Surgeon
Matthew Stiebel, MD FRCSC, is the newest partner at Palm Beach Sportsmedicine. After undergraduate and medical school degrees at Yale University, he completed an orthopaedic surgery residency at McGill University and a subspecialty fellowship in sports medicine at Boston University. His specialties include complex shoulder and knee injuries. Dr Stiebel has published papers and book chapters on specialty surgeries of the knee and shoulder. He is an associate master instructor for the Arthroscopy Asscociation of North America, where he instructs both arthrocopic shoulder and patellofemoral knee courses for surgeons in the US and internationally. He has lectured to the International Patellofemoral Reseach Group in London and New York City, and has worked with patellofemoral implant design companies. His other current interest involves the repair of pectoralis major muscle tears and their subsequent outcomes. While in Montreal, Dr Stiebel worked with the Montreal Canadians Hockey team and Expos Baseball team. During his fellowship time in Boston he was able to serve as team physician for the NCAA championship BU men’s hockey team, UMASS Boston Hockey, as well as work with the World Wrestling Entertainment Summer Slam Series. Locally, Dr Stiebel stays active in the community by currently serving as team physician for some of the local high school football and gymnastics programs.
Certificates/Memberships:
– Board Certification: American Board of Orthopaedic Surgery, July 2012
– American Academy of Orthopaedic Surgeons
– Fellow, Royal College of Physicians and Surgeons of Canada American Arthroscopy Association of North America
– International Society of Arthrosocopy, Knee Surgery & Orthopaedic Sports Medicine
– International Patellofemoral Reseach Group
Palm Beach Sportsmedicine
(561) 845-6000 | www.pbsportsmed.com
 South Florida Health and Wellness Magazine Health and Wellness Articles
South Florida Health and Wellness Magazine Health and Wellness Articles